Gut–Thyroid Connection: Why Bloating Is Common in

She is usually in her late 30s or early 40s. Her thyroid reports are described as “borderline,” or “stable.” Yet, by afternoon, her abdomen feels tight and uncomfortable. Meals leave her bloated than nourished. Constipation is common, and bowel movements feel incomplete. Alongside this are fatigue, mood swings, unexplained weight gain, and a persistent sense of something not being right. She says, “I am doing everything I have been told, but my body still feels off.”
This experience is extremely common in people with hypothyroidism. And it is not imagined. Bloating and thyroid symptoms are closely linked to what is known as the gut-thyroid connection.

Why Bloating and Thyroid Problems So Often Occur Together
Thyroid disorders, particularly hypthyroidism, are increasingly common, especially in women. Digestive complaints such as bloating, gas and constipation are equally widespread. Their frequent coexistence is not coincidental - it is physiological.
The thyroid and the digestive system are metabolically connected. When thyroid hormone signaling slows, digestive function slows with it. However, standard medical care often evaluates these systems separately. Thyroid health is assessed through blood tests such as TSH and T4, while digestive symptoms are commonly labeled as IBS, stress-related or functional issues.
Standard care prioritizes normalizing lab values and prescribing hormone replacement. What is often overlooked is how effectively thyroid hormones act at the tissue level - particularly in the gut. Gut motility, digestion, immune activation, inflammation, micronutrient deficiencies and chronic stress physiology frequently go unassessed. As a result, patients are told their thyroid is “normal,” while bloating and constipation persist.
How Hypothyroidism Disrupts Digestion
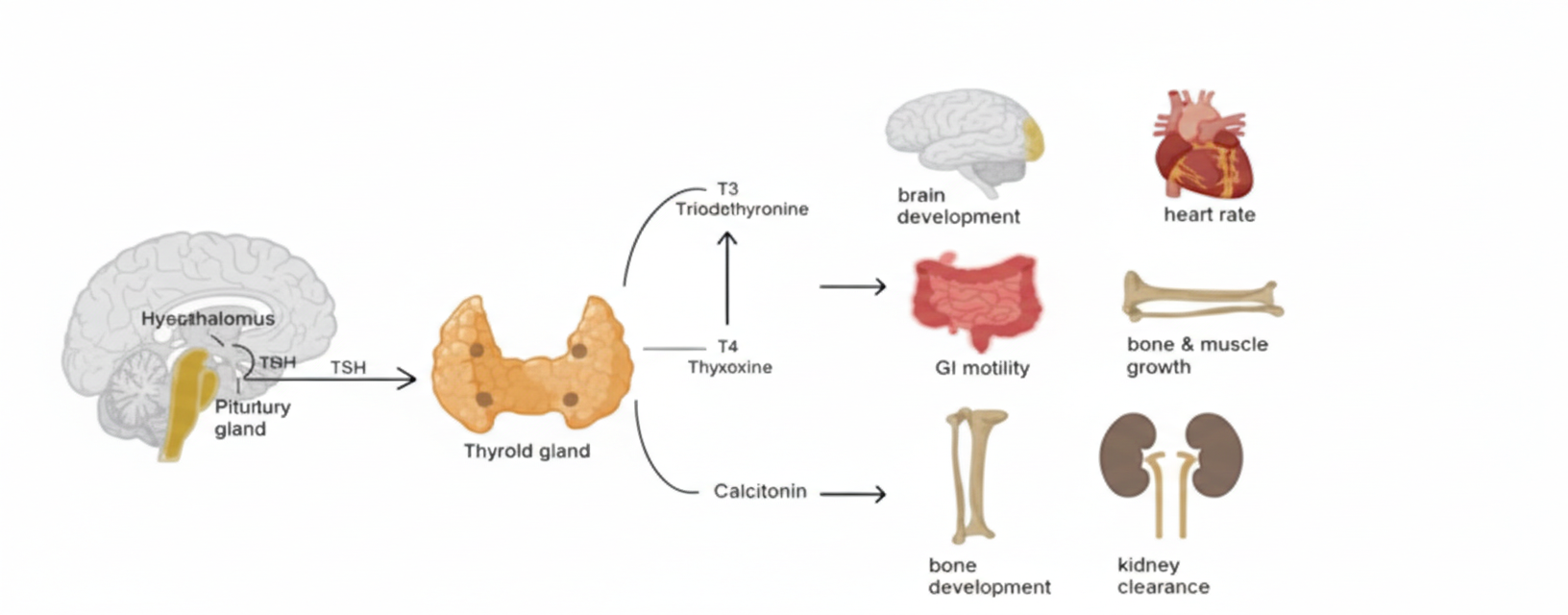
Thyroid hormones regulate metabolic speed throughout the body, including the gastrointestinal tract. In hypothyroidism, digestion slows. Intestinal muscle contractions weaken, stomach emptying is delayed, and bile flow becomes sluggish. Food remains in the gut longer than it should, increasing fermentation and gas production.
Clinically, this presents as bloating after meals, abdominal distension, excess gas, and constipation or incomplete bowel movements. There is also a deeper mechanism involved. A significant portion of thyroid hormone activation and recycling occurs in the gut. When gut health is compromised, T4 to T3 conversion is impaired, inflammation increases, and immune signaling becomes dysregulated.
This creates a reinforcing cycle: hypothyroidism slows digestion, poor digestion worsens gut health, and gut dysfunction further impairs thyroid hormone action. In this context, bloating is not a minor digestive issue—it is a marker of reduced metabolic activity in the gut.
Clinical Patterns Seen in Practice
Certain patterns appear repeatedly in clinical practice. Patients commonly present with persistent bloating, especially after meals, along with constipation, fatigue disproportionate to activity, weight gain resistant to calorie restriction, brain fog, low motivation, cold intolerance, and menstrual or perimenopausal irregularities.
Symptoms vary significantly between individuals. Two patients with similar thyroid blood values may feel entirely different. This variation depends on factors such as cellular thyroid hormone sensitivity, gut microbiome composition, immune activation or autoimmunity, micronutrient status, and stress-related nervous system regulation.
This variability explains why bloating often persists even after thyroid medication is started. While medication may normalize lab values, it does not automatically restore gut motility, digestion, or immune balance.
Why Isolated Treatment Often Falls Short
When bloating continues despite “normal” thyroid reports, deeper assessment is required. In my clinical approach, the thyroid is never evaluated in isolation. Instead, multiple interconnected systems are assessed together, including digestive function and gut motility, liver health and bile flow, micronutrient availability, immune and inflammatory burden, and stress physiology.

Treating only the thyroid hormone often results in partial or temporary improvement. Treating digestion without understanding thyroid signaling is equally limited. These systems are interdependent, and sustainable improvement occurs only when they are addressed together.
What Healing Really Looks Like
Restoring balance between the gut and thyroid is a gradual process. These systems are adaptive and are often dysregulated for years before symptoms become obvious. Healing tends to occur in phases rather than suddenly.
Patients should expect steady, progressive improvement rather than quick resolution, along with the need for consistency and periodic reassessment. Meaningful change typically unfolds over months, not weeks. This timeline reflects genuine physiological repair.
Timeframe for Healing
This approach is suited for individuals who experience bloating alongside thyroid symptoms, feel that standard reports do not reflect how they feel, want to understand root causes rather than suppress symptoms, and are willing to address multiple systems together.
It is not designed for quick fixes. It is for patients seeking clarity, structure, and sustainable recovery.
Who This Approach Is For
Bloating is one of the most overlooked manifestations of hypothyroidism. Addressing the gut–thyroid connection is essential for resolving digestive symptoms and achieving long-term thyroid health.
Clinical Takeaway

